And with a little help from hot cross buns
As a Clinical Psychologist, I often hear a misconception that we psychology types only want to consider interventions of the mind when trying to understand a client problem. In other words, we are only interested in thoughts and emotional feelings and how they impact behaviours, and that physical components remain the sole focus of medical and physical-based therapies.
We actually think more than you might believe or know about the body, physical sensations and the mind-body duality. We are, after all fans of the Biopsychosocial movement. And this has never been more true than in understanding pain and how to manage it effectively.
Cognitive Behavioural Therapy (abbreviated to the familiar CBT) is a commonly used treatment modality amongst Clinical Psychologists. We are heavily trained to use this approach effectively and there are a number of Third Wave ideas spinning off from its core principles (like Acceptance and Commitment Therapy and Compassion-Focussed Therapy). Psychologists apply CBT to a range of problems and pain management is no exception.
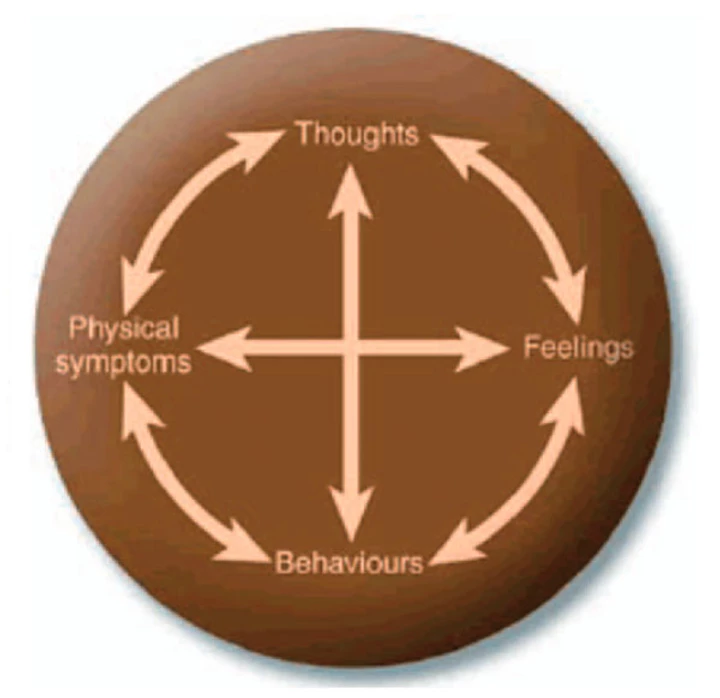
The basis of CBT is that of the ‘hot cross bun’ model, as shown above.
This model was developed by Christine Padesky in the 90s to help us formulate a problem by looking at four main parts of human experience:
· Thoughts
· Emotional feelings
· Behaviour
· Physical symptoms
You will see from the model that there are ‘mind’ components in Thoughts and Feelings. And ‘physical’ components in Behaviours and Physical sensations. You will also notice that they all influence one another, as denoted by the double-headed arrows. The interdisciplinarity of this model allows for the mind and body professionals to truly come together using the same conceptualisation to underpin their interventions.
So, an example of how this CBT model is applied in pain:
Thought: I think I will have a flare-up
Emotional feeling: Anxiety
Physical symptoms: I feel more pain
Behaviour: I avoid going out
In the same way these components are integrated, so should the treatment of pain: using both psychologists and physical health practitioners.
So, let’s see how this model looks in psychotherapy. A client might come to us with the following patterns:
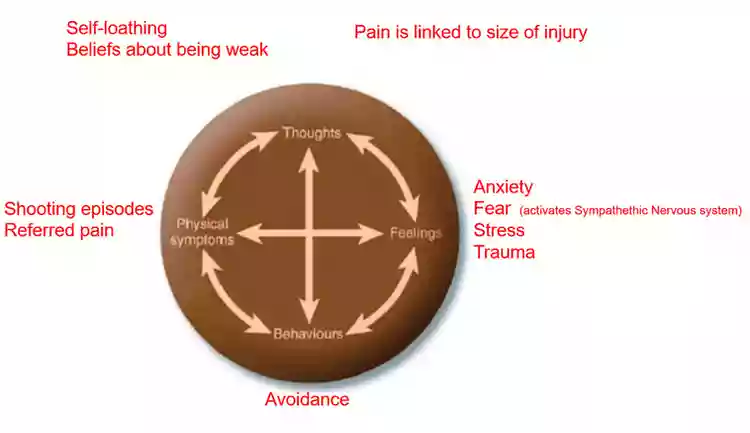
Thoughts: What we find when we enter the thoughts, there are lots of negative cognitive patterns that can be self-critical or that are based on untruths about what causes pain.
Feelings: When we look at emotions, we notice that stress and trauma come up a lot as the Sympathetic Nervous System is activated.
Behaviours: These feelings can lead to avoidance behaviours because humans have a natural instinct to run away from threat.
Physical symptoms: All these points culminate to increase the physical sensation of pain which in turn contributes to a negative downward spiral.
 What we would want to do instead is unpick those unhelpful patterns, or at least loosen it all up a bit:
What we would want to do instead is unpick those unhelpful patterns, or at least loosen it all up a bit:
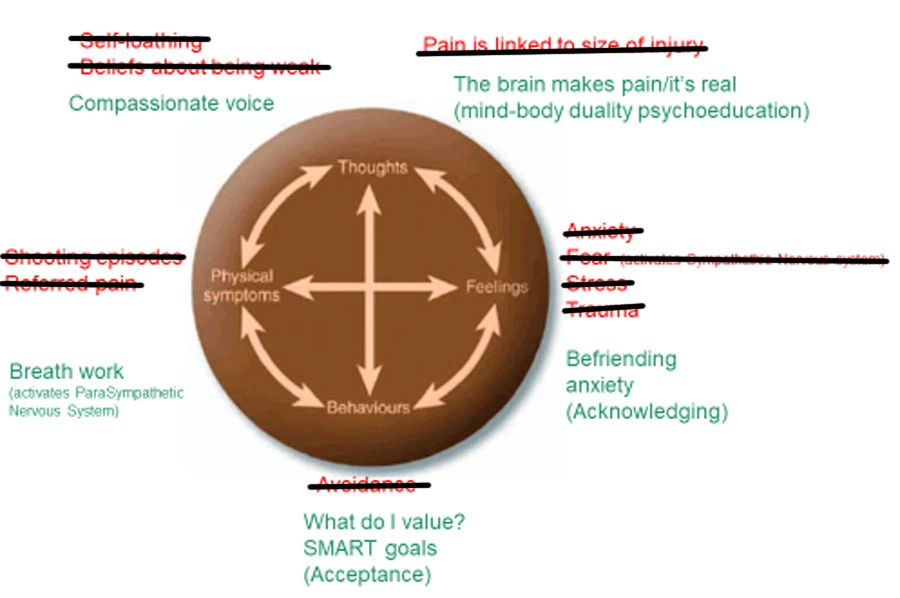
Thoughts: Thinking about how speaking to oneself gently, with loving kindness rather than beating ourselves up, and acknowledging the reality in the pain experience, despite there being no wound. Compassionate approaches are vital here.
Feelings: Reduce the sense of threat by befriending the pain. This is of course easier if your pain can be acknowledged by yourself and others including professionals so working with clinicians who can support how the mind and body work together is crucial.
Behaviours: Using Acceptance and Commitment Therapy ideas of underlying values that helps manage expectations about ourselves and what our life means now. What is your purpose and your aims? Are they SMART?
Physical symptoms: If we can activate the Parasympathetic Nervous System – the calming/soothing body system – we know pain can be reduced. With neuropathic pain that can sometimes shooting/instant, research says breathing is what our patients find most helpful. Mastering the breath can make the difference.
It is worth saying here that underlying these components is how we use language especially when working with people who do not speak English as a first language. Terms like ‘flare’ and ‘scans’ – even ‘goals’ – can be hard for some clients to remain neutral about, and so professionals who work with our pain clients need to consider what and how they speak within their roles.
So, to sum up:
• Psychoeducation: Mind-body connection is key to understanding pain and its management. A traditional medicalised approach is unlikely to work optimally for our clients and the system around our clients can learn this.
• Breath work should never be under-estimated. Certainly for neuropathic pain, it is all our clients have in their specific pain episodes.
• Avoidance does not work!!! Befriending pain does!
• Compassion and Acceptance therapies – spin-offs from CBT – are showing promising according to the pain research literature.
• Thinking about our use of language and its impact on emotions, especially for our non-native communities is a must from the consultants through to support workers to families/informal supporters.
• Consider interdisciplinary pain management ideas from the start when pain is part of the client’s presentation. Not part-way through, and not without strong conceptualisation like CBT as a guide. Only then is the outcome likely to be greater than the sum of its parts.
• Listen to The Psychology of Case Management podcast for more information on pain management, Acceptance and Compassion approaches and understanding the breath by experts in the field – www.psychworks.org.uk/podcast
Join our mailing list for free resources on working psychologically with Personal Injury clients to maximise rehabilitation and settlement outcomes: www.psychworks.org.uk/psychworks-presents
We also have free online resources via our Case Managers’ LinkedIn group and Personal Injury Professionals Facebook group to help you develop ideas to support your clients and be supported in your role.